Understanding Hives: Causes, Symptoms, and Treatment Options
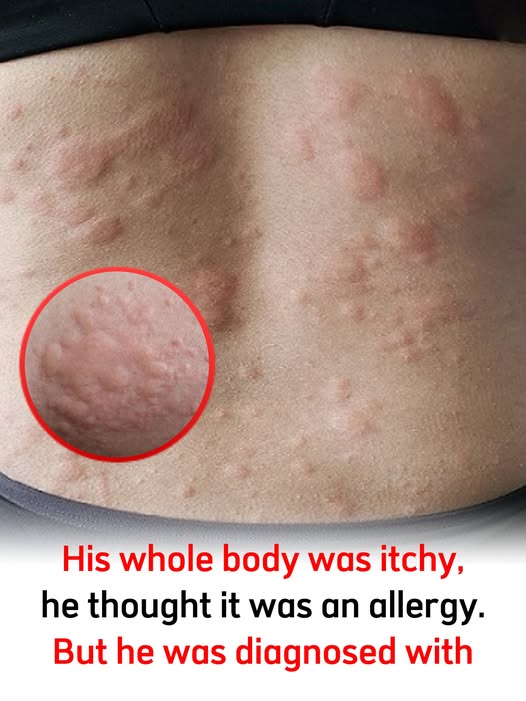
Hives, medically known as urticaria, are a common yet often misunderstood skin condition characterized by itchy, raised welts that can appear abruptly on various parts of the body. The welts may present in shades of pink, red, or flesh tones, particularly noticeable on lighter skin, while those with darker skin may notice darker variations. These welts can cause significant discomfort, often resulting in stinging or painful sensations that can disrupt daily activities and sleep. While many instances of hives are transient and manageable, they can also indicate underlying health issues, especially when they persist over time or recur frequently. Understanding hives is vital for effective management and improving one’s quality of life.
What Triggers Hives?
The appearance of hives is most frequently linked to allergic reactions. When a person encounters an allergen, their immune system responds by releasing histamines into the bloodstream. Histamines are chemicals that play a vital role in the body’s defense mechanisms, yet in some individuals, they can trigger the swelling and itching characteristic of hives. Common allergens include certain foods such as peanuts, shellfish, eggs, and dairy, as well as medications like penicillin and sulfa drugs, pollen from plants, insect stings, and pet dander. However, the triggers for hives extend beyond just allergens. Non-allergic factors can also provoke outbreaks. For example, extreme temperatures—whether hot or cold—can lead to the abrupt appearance of hives. Stress, an oft-overlooked factor, has been shown to exacerbate skin conditions, including hives, by triggering the release of cortisol and other stress hormones. Physical exertion, particularly intense exercise, can also be a contributing factor. Individuals may find that wearing tight clothing or excessive sweating can aggravate these skin reactions, leading to an outbreak. The wide array of potential triggers makes it particularly challenging for both patients and healthcare providers to pinpoint the exact cause of hives in many cases.
Risk Factors: Who Is Most Affected?
Certain demographics are more susceptible to developing hives. Individuals with a history of allergies, whether to specific foods or environmental factors, are at a heightened risk. This includes those with conditions like hay fever or asthma, as these individuals often have more reactive immune systems. Additionally, people undergoing medical treatments or taking medications known to induce allergic reactions may also experience hives. Chronic illnesses such as autoimmune disorders and infections can further compromise the immune system, increasing vulnerability to hives. Interestingly, women are statistically more likely than men to develop chronic hives, and cases often arise in young adulthood or middle age.